If you are asked to do a dental assessment on a patient would you know what to do? Here’s a quick overview on how to perform a thorough dental assess on a conscious patient. Obviously make sure the patient is amenable before attempting!
- Check for Temporomandibular Joint Function
Check the temporomandibular joint (TMJ) function by opening and closing the mouth. The TMJ is really a “hinge joint” where the mandible pivots between the open and closed positions. If there are issues with the TMJ, the occlusion, and opening/closing of the mouth may be affected. These issues are usually painful and will present with the jaw locking into an open or closed position. It is also good to note any popping or clicking noises or crepitus with in the TMJ.
- Look at symmetry
Compare both sides of the patient’s jaw and face to assess symmetry. Sometimes there are asymmetrical malocclusions present, where just one side of the maxilla and mandible don’t line up correctly, but the opposite side does. Or where the midline alignment of the maxilla and mandible aren’t in line.
In comparing one side to the other you may notice a thickening of a jaw or mandible, or swelling (for example) that isn’t obvious when examining independently.
- Palpation
Palpation of the face and jaw may reveal firm or fluid masses. Also palpate lymphatic and salivary tissue as abnormalities found may be related to intraoral disease. Palpation of the mandibles may reveal fracture or symphysial instability. The symphysis of the cat and dog refers to the fibrous union between the left and right mandibles.
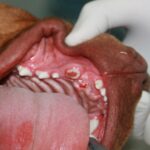
- Look inside oral cavity
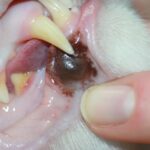
Look inside the patients mouth as best you can without getting bitten or scratched. The oral cavity is a common place to find neoplastic growths. These can be benign or quite malignant and the only way to know for sure is via biopsy. Caudal stomatitis could be described as a severe immune-mediated reaction to dental tissues.
- Oral Neoplasia
The oral cavity is the fourth most common place to encounter neoplastic growths. They range from very benign to quite malignant. The only way to know for sure what type of growth is present is to perform a biopsy.
- Assess Occlusion
Essentially you are trying to determine if the patient’s bite is right. Is the occlusion normal when the mouth is closed? This is more easily done when a patient is anaesthetised, however a quick assessment can be done in a conscious exam. For a normal occlusion the upper incisors overlap the lower incisors, with the tips of the lower incisors resting on the upper incisors. The lower canines should fit into the diastema (space) between the upper canines and the adjacent third incisors without contact between any teeth. The upper and lower premolars should interdigitate, with the lower premolars positioned rostral to the upper opposing teeth.
- Malocclusions are where the teeth don’t line up correctly. This can occur as a result of trauma or normal genetics. There are 3 types of malocclusions commonly seen:
- Neutroclusion – This is where the jaw lengths are normal, but one or more teeth are in an abnormal position. Examples include rostral crossbite and caudal crossbite.
- Mandibular distoclusion – This is commonly known as an underbite where the mandible resides caudal to its normal location in relation to the maxilla.
- Mandibular mesioclusion – The is also known as an overbite were the mandible resides rostral to its normal location in relation to the maxilla. This is commonly seen in brachycephalic breeds.
In some cases, the patient may only have a temporary malloclusion. In these cases, the alignment problem is typically mild. These temporary malocclusions occur when the maxilla and mandible grow at varying rates during development due to an independent jaw growth surge.
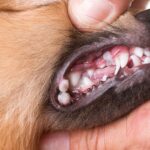
- Count the teeth
It is recommended to count the patient’s teeth, as this helps to determine if there are missing or extra teeth. Normally dogs will have 42 permanent teeth, whilst cats have 30.
- Persistent deciduous (baby) teeth are very common, especially in small and toy breed dogs. They occur when the baby teeth don’t fall out before or when the adult teeth come through, resulting in two teeth occupying the one spot! If the retained baby teeth are left in place they will create problems and should be treated promptly.
- Feline Tooth Resorption occurs when cells called odontoclasts destroy the tooth root surfaces and cause the enamel to be resorbed. As the disease progresses, the different layers of the tooth are resorbed and the pulp cavity becomes exposed, causing pain and sensitivity. The resorption continues until the tooth is weakened and ultimately fractures. Since, these lesions usually start at the gum line, they are often covered with gum tissue or tartar and therefore may be difficult to detect without a thorough oral examination.
- Missing Teeth occur for a variety of reasons including: congenitally missing, previously extracted, fractured (or extracted) with retained roots, or impacted teeth. Dental radiographs are necessary to assess the cause and would be recommended if the patient is undergoing a general anaesthetic. If dental radiographs reveal retained roots and evidence of inflammation or infection (clinical or radiographic) is detected, then the teeth should be surgically extracted.
- Check teeth for fractures or any other anomalies
Coronal defects may involve: only the enamel, both the enamel and dentin “near pulp exposure,” or direct pulp exposure. Teeth with coronal defects often have rough surfaces with accumulations of plaque and calculus.
The carnassial teeth are frequently chipped or fractured in dogs that are allowed to chew hard objects. Caged animals with separation anxiety frequently incur defects or fractures on the distal surfaces of incisors, canines, and premolars, sustained when trying to escape from their cages.
Dogs that habitually carry tennis balls develop severe dental abrasion. Dental attrition results from abnormal coronal wear due to excessive mastication or chewing.
Slab fracture of a carnassial tooth frequently results in suborbital swelling. However, dental radiography should be performed before extracting the fractured tooth to ensure accurate diagnosis and treatment of the tooth or teeth causing the swelling. Tooth root abscess of the upper third premolar or upper first molar, foreign body penetration, and infectious or neoplastic diseases can also cause swelling and must be ruled out via dental radiography. Lingual fractures of the lower first molars are also common but are often missed during routine oral examination.
- Soft Tissue Evaluation
Assess all four dental quadrants for normal gingival colour and anatomy. Gingival defects, recession, discolouration, inflammation and oedoma may also be evident. Since the gingiva protects the teeth and other periodontal structures, its loss creates a risk for periodontal disease progression, endodontic disease development and the eventual loss of adjacent teeth.
- Assess the amount of plaque
Plaque is the colourless film that constantly forms on teeth. If it is not regularly cleaned off it will build up into calculus or plaque. Use a plaque disclosing solution to check for the amount of plaque on the teeth.
Here is a quide to assess plaque:
PI-0: No plaque
PI-2: Minimal
PI-2: Moderately dense
PI-3: Heavy plaque deposits
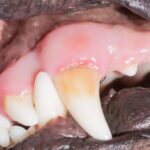
- Assess the level of calculus on the teeth
If calulcus is left it will build up significantly and can cause many problems for the patient.
Here is a guide to assess calculus:
CI-0: No calculus
CI-1: Minimal supragingival (above the gingiva and on the tooth) calculus deposition
CI-2: Moderate subjingival (beneath the gum, and around the base of the tooth) and supragingival calculus deposition
CI-3: Heavy calculus deposits on crown and subgingivally
- Assess the amount of gingival inflammation,
Gingivitis, which is evidenced by a reddening of the gums directly bordering the teeth, is considered to be an early stage of periodontal disease. It can be caused by a build up of plaque or calculus that builds up on the teeth and irritates the gum.
A guide to gingival assessment is:
G1-0: Normal gingival shape and colour
G1-1: Mild gingival inflammation, swelling, slight red colour
GI-2: Moderate gingival inflammation, swelling, red with bleeding
GI-3: Server gingival inflammation, swelling, bright red with bleeding
A quick note on Periodontitis
Stage 1 – Gingivitis
- Margin of attached gum (gingival) is inflamed and swollen
- Plaque covering teeth
Stage 2 – Early Periodontitis
- Entire attached bum is inflamed and swollen
- Mouth is painful and odour begins to be noticeable
Stage 3 – Moderate Periodontitis
- Cherry red and bleeding attached gum is being destroyed by infection and calculus.
- Sore mouth affects eating and behaviour
- Bad breath is present
- Beginning of periodontal disease
Stage 4 –
- Chronic bacterial infection is destroying the gum, tooth and bone.
- Bacteria may be spreading throughout the entire body via the bloodstream